What Good Healthcare Data Looks Like (And Why Most Organizations Don’t Have It)
Healthcare organizations generate a large amount of data every day, including patient interactions, referral activity, outreach campaigns, and care coordination touchpoints, just to name a handful of common examples. But having data is not the same as having useful data. In many cases, teams are working with incomplete, inconsistent, or disconnected information that limits their ability to make decisions. The gap between data volume and data quality is one of the most underappreciated challenges in healthcare operations.
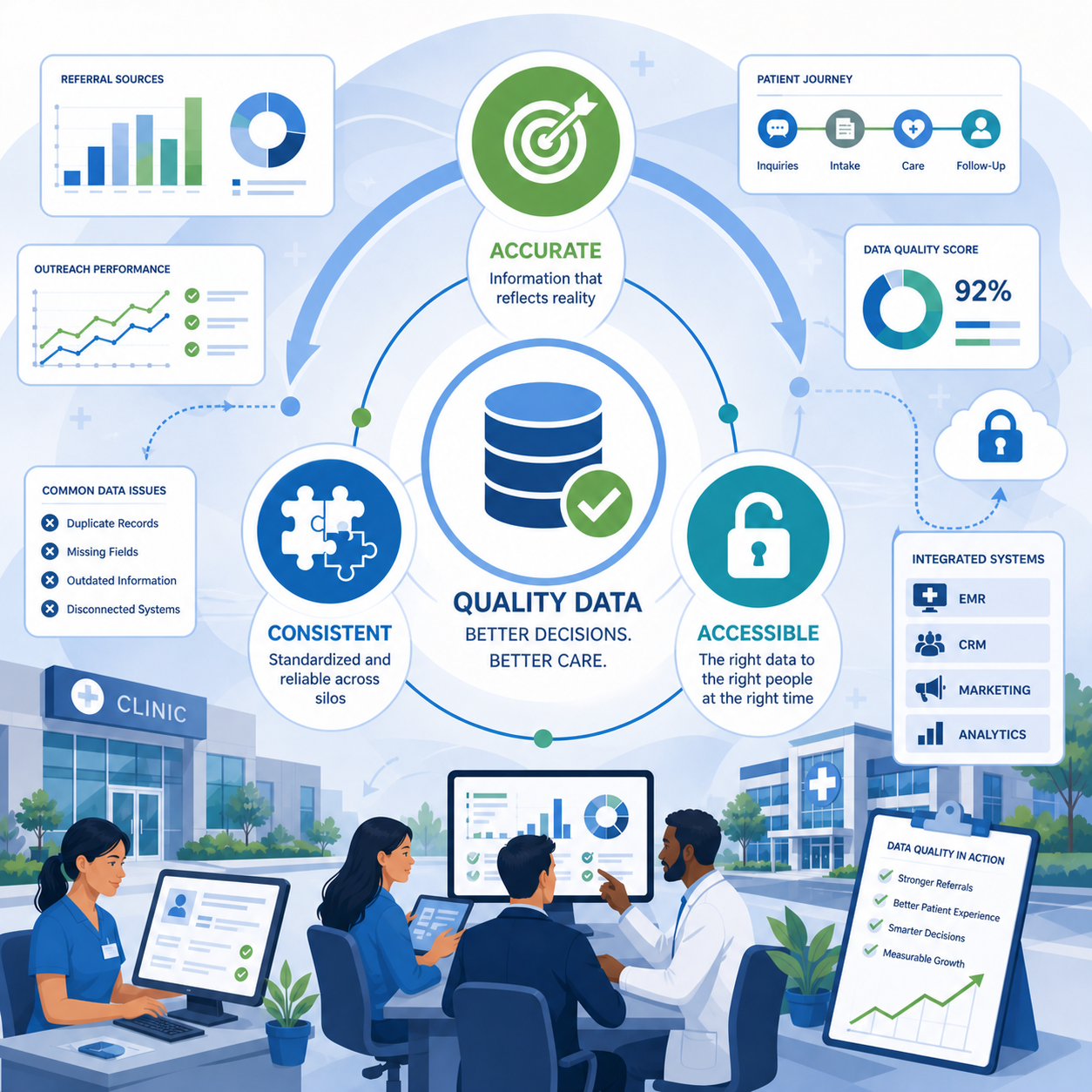
Good healthcare data has three key qualities. Generally speaking, it should be accurate, consistent, and accessible.
Accuracy means the information reflects reality. Patient records are complete, referral sources are correctly attributed, and every outreach interaction is properly logged. Inaccurate data leads to missed follow-ups, poor reporting, and lost referral relationships. It can also undermine credibility when clinical or administrative leadership can't trust the numbers in a report, and they default to gut instinct instead of evidence-based decision making.
Consistency means data is entered and managed the same way across systems, care sites, and teams. Without standardization, reports become unreliable. One clinic or service line may track patient inquiries differently than another (extremely common across MSO practices), making it difficult to compare performance or identify trends across the organization or portfolio. Consistent data entry practices are the foundation of any meaningful analysis, whether you're measuring referral conversion rates, campaign ROI, or patient acquisition costs.
Accessibility means the right people can easily access the data they need, when they need it. If patient and referral information is spread across disconnected EMRs, CRMs, and spreadsheets, teams spend more time searching than acting. In fast-moving healthcare environments, delays caused by inaccessible data can have real consequences for both operational efficiency and the patient experience, dragging down both unnecessarily.
Most healthcare organizations struggle with at least one of these areas. Common issues include duplicate patient or referral records, missing intake fields, outdated physician contact information, and CRM or EMR systems that do not integrate well. Over time, this erodes trust in the data. Teams stop relying on it and fall back on assumptions about which referral sources are performing or which campaigns are driving volume. What begins as a technical problem gradually becomes a cultural one, and reversing that mindset can be more expensive to fix than even the original investment.
Improving data quality requires a structured approach. Start by defining clear standards for how patient, referral, and outreach data should be captured and maintained across every touchpoint. Document those standards in a way that is practical and accessible to the people doing the work, such as front desk staff, care coordinators, and marketing teams, and not just the administrators who designed the systems. Then implement processes to ensure those standards are followed consistently.
Regular audits are also important. Reviewing records for errors, gaps, and duplicates helps maintain quality over time. These audits don't need to be exhaustive to be effective, as even a monthly review of key fields like referral source, patient status, and outreach history can catch issues before they compound. Training staff on proper data entry and usage is another critical step. People are more likely to follow standards when they understand the downstream impact. A missing referral source, for example, directly affects the organization's ability to measure and grow those relationships.
When data is clean and reliable, it becomes a powerful tool for healthcare growth. Organizations can track referral patterns, identify bottlenecks in the patient journey, and make informed decisions about where to focus outreach efforts. They can also respond more quickly to change, whether that means adjusting a campaign strategy, reallocating business development resources, or identifying shifts in referral behavior before they affect volume.
Good data does not happen by accident. It is the result of clear processes, consistent execution, and ongoing attention. For healthcare organizations looking to grow their patient population, strengthen referral networks, or demonstrate marketing ROI, investing in data quality is not a back-office concern, but should be a strategic priority.